Improvements in imaging technology,
endoscopic equipment, drug treatment, and scientific innovation have all contributed to recent advances in
gynaecology. Advances have also resulted from a change in the attitudes and practice of gynaecologists themselves, in response to the greater expectations and knowledge of their patients, who frequently seek new and innovative procedures on the basis of media publicity and access to non-peer reviewed information including the world wide web. It is increasingly recognised that
gynaecological problems affect the quality of life of women in different ways, highlighting the value and importance of patient assessed health status measures to evaluate the subjective severity and treatment efficacy of common gynaecological conditions.
Laparoscopic and
hysteroscopic surgery, medical treatment, and expectant management are replacing major gynaecological surgery for many common gynaecological complaints. For example,
ectopic pregnancy is being diagnosed earlier by the use of transvaginal ultrasonography and quantitative measurements of human chorionic gonadotrophin concentrations. Thus women can be treated either medically as outpatients with methotrexate injections3 4 or by laparoscopic surgery, reducing stay in hospital and preserving tubal function in most cases.4–6 Minor procedure units for gynaecology, with one stop investigation and treatment (including ultrasonography and hysteroscopy), and early pregnancy assessment units, where
bleeding in early pregnancy can be dealt with rapidly and sympathetically, are becoming more commonplace. The prolonged life expectancy of menopausal women and their higher expectations for health have encouraged new developments in hormone replacement therapy. The increased use of such therapy has also increased surveillance and thus recognition of other common problems affecting older women. Delaying childbearing has resulted in a greater demand for effective fertility treatments and for surgical procedures that preserve fertility.
Methods:
We asked consultant gynaecological staff at a London teaching hospital for their views on important recent advances in gynaecological practice. Overlap occurred in topics believed to be important, and these are detailed here. To supplement our knowledge of the relevant recent literature, we electronically searched Medline, hand searched the major British and US gynaecological journals published over the past 2 years, and read presentations and abstracts from the 1998 British congress of obstetrics and gynaecology.
Treatment of menorrhagia
Hysterectomy:
Heavy
menstrual loss is a common complaint and accounts for about 12% of referrals to gynaecology outpatient departments. Many of these women will undergo
hysterectomy—a woman’s lifetime risk of hysterectomy is estimated at 20%. Despite the success of the procedure compared with other treatments for
menorrhagia, the morbidity and complication rates (before and after discharge from hospital) are high. The frequency of the operation and its complications have provided incentives to re-evaluate simple medical treatment and to explore new conservative and surgical treatments for dysfunctional
uterine bleeding.
Medical treatment Randomised controlled trials of commonly prescribed medical treatments for menorrhagia have confirmed the efficacy of
tranexamic acid and have shown that norethisterone, the most commonly prescribed drug in the United Kingdom for the treatment of
ovulatory menorrhagia, is ineffective at its recommended dosage. Despite this evidence, a recent survey of 206 general practitioners showed that 69% would still consider prescribing cyclical norethisterone for this condition. Even when used appropriately simple medical treatment may not relieve the symptoms of menorrhagia. Although this may result from inappropriate prescribing, evidence from studies of patient satisfaction and quality of life have shown that women with severe self assessed symptoms are unlikely to experience improvement with
drugs.
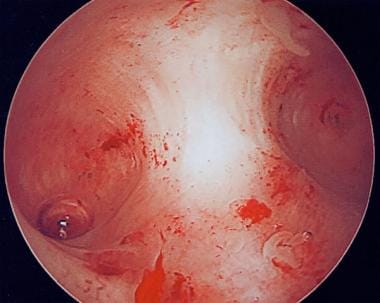
Hysteroscopic ablative surgery:
If medical treatment fails to treat menorrhagia, an alternative treatment is hysteroscopic ablation of the
endometrium. Several techniques are available, and despite initial concerns about safety a recent survey of more than 10 000 operations (MISTLETOE; miminally invasive surgical techniques, laser,
endothermal or endoresection) showed that the techniques are safe even in inexperienced hands. At the start of the survey in 1993, 83% of NHS hospitals in the United Kingdom offered ablative surgery. Although randomised trials have shown ablative surgery to be more effective than medical management, the technique is invasive, requires general
anaesthesia, is not without complications, and has reduced long term efficacy in women under 45 years of age.Recently introduced balloon devices for ablative treatment may prove to be equally efficacious, simpler, and even safer to use than ablative surgery, although further evaluation is awaited.
The hysteroscopic resection of small submucous fibroids distorting the endometrial cavity is now standard practice , but not all fibroids are amenable to this surgical option because of their position and size. In the presence of large symptomatic fibroids, hysterectomy or
myomectomy has remained the major treatment option. Recent advances in the long term interventional radiological and medical treatment of large symptomatic myomas offer an important alternative approach.

Although the gonadotrophin releasing hormone agonists are more frequently used in assisted
conception, in the management of endometriosis, for the premenstrual syndrome, and to prepare the endometrium before
hysteroscopic surgery, they have also been shown to reduce the size of fibroids by up to 50% with short term treatment (3-6 months). This has made them an ideal adjunct to surgery for large symptomatic fibroids. The main disadvantages of
gonadotrophin releasing hormone agonists are secondary to the induced hypooestrogenic state, affecting the cardiovascular, skeletal, and urogenital systems and producing vasomotor symptoms. This has limited their use to short term treatment, the cessation of which leads to a rapid increase of fibroids to their previous dimensions. Thus the short term treatment of fibroids with gonadotrophin releasing hormone agonists alone is a costly and ineffective treatment option.
Overcoming male factor infertility:
It is now 21 years since the first live birth after fertilisation in vitro to alleviate female tubal infertility. Despite only moderate success (between 9% and 26% live births per cycle started), influenced mainly by maternal age, duration of infertility, and previous parity, in vitro fertilisation is now accepted as an alternative to tubal surgery and for protracted unexplained infertility. In a similar way, the recent ability to achieve
fertilisation of eggs in vitro by the injection of a single spermatozoon (intracytoplasmic sperm injection; ICSI) has overturned the poor prognosis for men with low sperm counts or azoospermia. Adequate spermatozoal samples for intracytoplasmic sperm injection can be obtained from very poor ejaculates, including semen samples frozen for patients undergoing
chemotherapy or radiotherapy but too poor to be used for artificial insemination. In men with obstructive azoospermia of infective origin or after failed reversal of vasectomy, sperm for intracytoplasmic sperm injection can be obtained by percutaneous aspiration from the epidydimis (PESA) or from a small testicular biopsy (testicular sperm extraction; TESE), performed under local anaesthesia. This latter technique may be used in men with small testes and a high follicle stimulating hormone concentration who have testicular failure, as multiple small biopsies will show adequate sperm for intracytoplasmic sperm injection in half the cases. Pregnancy success with intracytoplasmic sperm injection is as good as or even better than with in vitro fertilisation, and the outcome seems to be independent of the source of the sperm.








